Caregiver Self-Care And Stress Management
Managing your Care when Caring for Others
Caregivers who care for individuals with Alzheimer’s or Dementia should manage their stress to prevent burnout and keep their caregiving optimism high.
Challenges involved in caring for someone with these and other conditions. Caring for individuals with Alzheimer’s or dementia can cause special challenges for the caregiver
COMMUNICATION
Communication can be especially challenging between the caregiver and patient. Because an individual with Alzheimer’s or dementia may not remember names, conversations or events, they may repeat questions, have difficulty finding the right words, easily lose their train of thought and speak less frequently.
BEHAVIORS
Individuals with Alzheimer’s or dementia can exhibit behavior changes including depression, agitation, aggression, confusion, and suspicion. Caregivers can remain calm and patient and accept behaviors as a part of the disease in order to better work through it.
MEMORY LOSS
Memory loss may be mild in the early stages, but as the disease progresses, so will the level of memory loss. Caregivers can be called the wrong name, not be recognized, and more as individuals lose their memory.
Managing Caregiver Stress
Providing care for individuals in these and other conditions can be extremely fulfilling and challenging at the same time. It’s important that caregivers take care of themselves so they can remain hopeful, energetic and optimistic to provide proper care.
Signs of Caregiver Stress (womenshealth.gov)
- Feeling overwhelmed, frustrated and angry
- Making mistakes when giving care
- Feeling alone, isolated, or deserted
- Not getting enough sleep
- Getting too much sleep
- Gaining or losing a lot of weight
- Feeling tired frequently
- Losing interest in activities you used to enjoy
- Becoming easily irritated
- Feeling constantly worried or sad
- Having headaches or body aches often
Self-Care and Stress Management Tips
It’s important for caregivers to take care of themselves, both physically and emotionally even while they care for others. Finding the time to care for yourself with proper nutrition, exercise, and sleep—as well as getting support from family and friends will help caregivers relieve stress and can prevent burnout.
Physical Ways To Manage Stress
- Get regular exercise
- Participate in extracurricular activities
- Eat a balanced diet
- Pamper yourself
- Meditate
- Stay on track of your own health
- Get plenty of sleep
- Get regular doctor check ups
- Mental/Emotional ways to manage stress
- Talk with supportive friends
- Get support from family members
- Celebrate small victories
- Applaud your own efforts
- Enjoy a good laugh
- Join a caregiver support group
- Get help when you need it
- Set routines and stay organized
Home Care Tip:
There are many community resources available for caregivers such as adult day care programs, in-home assistance, and meal delivery programs. Contact the Alzheimer’s Association or use this (alz.org/CRF) Resource Finder to locate dementia care resources near you.
- Published in CAREGIVERS, IN HOME CARE
4 TIPS FOR CARING FOR AGING VETERANS
How to Care for our Veteran Population
Caregivers can help enhance the quality of life for veterans by advocating on their behalf and helping them find services for their unique needs.
Veterans have sacrificed everything to protect and serve our country. They have served in conflicts around the world for the freedoms that we have today. It is essential that veterans are cared for both physically and mentally, both during and after their time in the service. Throughout the duration of their lives, we should continue to honor and care for them.
According to the 2012 U.S. Census brief (census.gov), there were more than 12.4 million veterans ages 65 and older. With veterans and the population in general having a greater life expectancy than in years past, it’s important that our care can help sustain the public services and special support that these individuals need.
1. Getting the right care
The type of care that veterans may need will vary and can include routine physical care, traumatic brain injury care, treatment for post traumatic stress disorder and other emotional needs, rehabilitation, nutritional and dietary needs, wound injury and trauma, and more. The diversity and uniqueness of the care is as diverse and unique as the individuals who have fought for our country.
2. Paying for care
The Department of Veterans Affairs (VA) provides benefits and services for a variety of issues that veterans face.
Compensation can include disability compensation, Special Monthly Compensation (SMC), Adapted Housing grants (benefits.va.gov), Service-Disabled Veterans’ Insurance (benefits.va.gov), Veterans’ Mortgage Life Insurance (benefits.va.gov), Aid and Attendance (A&A) and Housebound care (benefits.vs.gov), Extended or long-term care and geriatric care.
Much of this compensation is a tax free monetary benefit paid to veterans and/or their spouses, surviving spouses and parents. Which programs each Veteran qualifies for will depend on their unique circumstances.
3. Supporting Mental and Emotional Health
Many veterans need more than just physical care. They need mental and emotional care to help them in dealing with PTSD, depression, suicidal thoughts, hopelessness, anxiety and other issues.
The VA offers mental health care for veterans (mentalhealth.va.gov), and is committed to a recovery-centered approach. Veterans can receive primary care for mental illnesses or receive more intensive treatment in specialty mental health care if necessary.
4. Activities to increase quality of life
Caregivers can help improve the overall quality of life for veterans on a day-to-day basis by engaging with them in different activities.
- Allow them to share stories: Ask veterans stories about when they were younger. Many of them will love to re-live tales from their past and share them with someone else.
- Let them give back: Although veterans have already given so much, it can be important for them to continue this spirit of giving to others. Find a place where they can volunteer. It can help boost confidence and give a sense of purpose.
- Help them find community: Military life has a built-in community and many veterans may miss that once they are no longer active. Help them find a group where they can connect with others and share similar experiences.
- Keep a routine: Many veterans are used to regimented routines and thrive off of schedules. Keep a regular routine each day and allow them to know the schedule. This can give them a sense of peace.
For years these veterans were advocates on behalf of us—whether it was directly or indirectly. We have all benefited from the sacrifices they have made. Caregivers can be their advocates by helping them navigate through various VA benefits, finding mental health solutions and doing daily activities with them that increase their quality of life.
Home Care Tip:
Caregivers should pay attention to veterans and what their individual needs are. Make sure to also recognize the abilities that veterans still have and to acknowledge those as well.
- Published in CAREGIVERS, IN HOME CARE
ALZHEIMER’S AWARENESS
National Alzheimer’s Disease Awareness Month: What Caregivers Should Know
Understand the three stages of Alzheimer’s disease and how caregivers can help patients in each of these different stages
Alzheimer’s or Dementia?
Alzheimer’s and dementia are often confused and used interchangeably, but they are different.
Dementia is an umbrella term that refers to a list of different symptoms, one of those being brain and memory function. There are diseases other than Alzheimer’s which can cause dementia. When an individual is diagnosed with dementia, they are being diagnosed with a set of symptoms, without knowing what is specifically causing them. Some forms of dementia are temporary or reversible. Alzheimer’s disease is a form of dementia that specifically affects parts of the brain that control thought, memory and language. Symptoms of the disease include impaired thought, speech and confusion. Alzheimer’s is not reversible or curable.
10 signs of Alzheimer’s (www.alz.org)
Here are 10 warning signs and symptoms of a person having Alzheimer’s disease.
1. Memory loss that disrupts daily life
This is the most common sign. Forgetting information that was recently learned, forgetting important dates or events, asking the same information over and over and relying heavily on memory aids or other people for reminders are all signs of Alzheimer’s.
2. Challenges in planning or solving problems Individuals with Alzheimer’s may have difficulty following a plan or
Individuals with Alzheimer’s may have difficulty following a plan or working with numbers. They may be unable to follow a familiar recipe, keep track of monthly bills, or have difficulty concentrating and carrying out simple tasks that didn’t present a problem before.
3. Difficulty completing familiar tasks People with Alzheimer’s may find it hard to complete tasks such as driving to a familiar location, managing a budget, or remembering the rules to a favorite game.
People with Alzheimer’s may find it hard to complete tasks such as driving to a familiar location, managing a budget, or remembering the rules to a favorite game.
4. Confusing time or place Losing track of dates, seasons and time is a common sign of Alzheimer’s. People with the disease may forget where they are or not know which day of the week it is. They could also have trouble understanding something if it is not happening immediately.
Losing track of dates, seasons and time is a common sign of Alzheimer’s. People with the disease may forget where they are or not know which day of the week it is. They could also have trouble understanding something if it is not happening immediately.
5. Difficulty understanding visual images and spatial relationships Experiencing vision problems can be a sign of Alzheimer’s. Some people may have trouble reading, judging distance and determining colors.
Experiencing vision problems can be a sign of Alzheimer’s. Some people may have trouble reading, judging distance and determining colors.
6. Trouble with finding the right words People with Alzheimer’s may have trouble finding the right words. They may call items or people by the wrong name. They might stop in the middle of a sentence and not know how to continue.
People with Alzheimer’s may have trouble finding the right words. They may call items or people by the wrong name. They might stop in the middle of a sentence and not know how to continue.
7. Misplacing things and losing the ability to retrace their steps Individuals with Alzheimer’s may lose items and be unable to retrace their steps to find them. They might put things in odd places. They may even accuse others of stealing.
Individuals with Alzheimer’s may lose items and be unable to retrace their steps to find them. They might put things in odd places. They may even accuse others of stealing.
8. Decreased or poor judgement Alzheimer’s can affect the decision-making process. Therefore, people with the disease may use poor judgement such as giving money away to telemarketers or solicitors.
Alzheimer’s can affect the decision-making process. Therefore, people with the disease may use poor judgement such as giving money away to telemarketers or solicitors.
9. Withdrawal from activities
A person with Alzheimer’s might start to avoid being social and may even withdraw from hobbies, social activities, or work projects. They may have trouble remembering how to complete a favorite hobby or keep up with a favorite sports team.
10. Changes in mood or personality
Someone with the disease can become confused, anxious, fearful or depressed. They can get easily upset.
The 3 stages of Alzheimer’s (www.alz.org)
STAGE 1 | MILD ALZHEIMER’S (EARLY STAGE)
In the early stages of Alzheimer’s, friends and family may start to notice
their loved one experiencing difficulty remembering things such as
familiar words or the location of everyday objects.
Common symptoms include:
• Difficulty finding the right word for something
• Forgetting something they just read
• Not remembering names of people they were just introduced to
• Difficulty performing routine tasks at work or socially
• Losing or misplacing objects
• Trouble planning or organizing
WHAT CAREGIVERS CAN DO AT THIS STAGE:
Since the individual is still independent at this stage, a caregiver’s’
role can be to provide support and companionship. The person with
Alzheimer’s may need help with things like:
• Appointments
• Managing finances
• Remembering names or words
• Transportation
• Planning and organizing
• Keeping track of medication
It’s important to allow the person to maintain their independence as
much as possible and keep communication open for when they do
need assistance.
STAGE 2 | MODERATE ALZHEIMER’S DISEASE (MIDDLE STAGE)
This is usually the longest stage and individuals can stay in this stage for
several years. As the disease progresses, the need and level of care will
become greater. People at this stage may start to confuse words, get
angry or frustrated or act out in unexpected ways.
Symptoms will be more noticeable and include:
• Forgetting information such as their own address or telephone
number
• Feeling moody or withdrawn, especially in socially or mentally
challenging situations
• Changes in sleep patterns
• Forgetting events about their own life
• Being confused on what day it is or where they are
• Needing assistance picking out clothes that are appropriate for the
season or occasion
• Urinary and bowel incontinence
• Wandering and getting lost
• Personality and behavioral changes, including suspiciousness
and delusions
WHAT CAREGIVERS CAN DO AT THIS STAGE:
Individuals at this stage will require a greater level of care. The person
with Alzheimer’s may become frustrated and upset when they have
difficulty remembering things and names or trouble with daily activities
such as getting dressed. You will most likely have to adjust your daily
routine to include more structure for the individual with Alzheimer’s. At
this stage caregivers can:
• Use a calm voice when responding to questions to help the
person from getting upset or frustrated.
• Respond to the person’s emotion, instead of the question asked.
The individual may need reassurance.
• If the individual can still read, write out reminders for them.
Practice patience and sensitivity with patients in this stage. They
may become increasingly upset or frustrated as they lose more brain
function as well as their independence.
STAGE 3 | SEVERE ALZHEIMER’S DISEASE (LATE STAGE)
In the final stage of Alzheimer’s, personality changes may occur and
individuals need increasing help with daily activities. They may still use
words or phrases, but communicating emotion becomes difficult.
Symptoms and behaviors at this stage may include:
• Changes in physical abilities, including the ability to walk, sit and swallow
• Needing assistance with daily personal care
• Not knowing their surroundings or recalling recent experiences
• Increasingly difficulty communicating
• Vulnerability to infections, particularly pneumonia
WHAT CAREGIVERS CAN DO AT THIS STAGE:
Intensive, around-the-clock care is usually required at this stage and can last
from several weeks to several years. The role of the caregiver is to preserve the
quality of life and dignity for the individual. People in this stage will need help
with most activities including eating, dressing, and even walking. At this stage,
the world is mainly experienced through the senses. Caregivers can connect
and help an individual by:
• Playing his or her favorite music
• Reading excerpts of their favorite books
• Looking at old photos with them
• Preparing a favorite meal
• Brushing the person’s hair
• Sitting outside together
Although an individual in this stage is unable to communicate, research shows
that some core of their self may still remain. Caregivers and loved ones may
be able to connect on some level even in this stage of the disease.
National Alzheimer’s
Disease Awareness Month
H E A LT H C A R E O B S E R VA N C E
Home Care Tip:
Home Care services can help help by reminding those with
cognitive impairment to take medications, eat, and drive.
- Published in ALZHEIMER
Senior Driving Safety
Should You Wait for an Accident to Take the Car Keys Away from Your Senior Parent?
Most adult children don’t know how to determine if their parent should be driving or not. Read more to find out if your senior parent is safe to be on the road.
How to Tell if Your Older Adult Parent is Safe to Drive
There is a moment that comes for nearly every senior and their loved ones: the day they decide that driving is no longer an option. This can be difficult for everyone involved, but if you notice your loved one’s senses are in decline, should you wait for an accident before you take the keys from the older adult in your life? The answer is usually “no.”
Why Are Seniors More Prone to Driving Accidents?
No one wants to give up their independence, but you may actually be helping your older parent live a longer, safer life by restricting their driving privileges. The truth is, seniors over age of 65 are almost twice as likely to die in car accidents than in any other type of accident. In fact, 15 older adults die in car accidents every day and 586 are injured daily. In addition, seniors are more likely to cause an accident. This is especially true over the age of 70. Between the ages of 70 and 74, there is a spike in car accidents. Seniors over the age of 85 have even more accidents – and they tend to be more serious. The reasons for this is due to increased susceptibility to medical complications and injury. Also, seniors tend to cause more accidents due to decline in vision and cognitive function. Medications can also play a part in the increase in accidents as they can cause impairment in drivers.
How to Decrease Chances of Accidents Behind the Wheel
While the statistics may sound discouraging, there are ways to reduce the chance of a senior you love having an accident:
- If possible, avoid medications with side effects.
- Plan your route before driving.
- This will help avoid confusion later on.If you need glasses or corrective lenses, wear them.
- And consider anti-reflective coatings to help minimize glare.
Finally, one of the best ways to decrease the chance of an accident is to not drive at all. With today’s home care options, a senior can use the aid of a home caregiver to run errands and drive to appointments and other outings. If your loved one has poor vision, has arthritis or a condition that makes it difficult to turn their head, having a home care aid assist with transportation to appointments, grocery runs, and to stay active and connected in the community can be a great idea. While it’s sometimes difficult to have the conversation about driving with your loved one, don’t wait until something happens. Now is the time to do so. You’ll be glad you did.
- Published in CAREGIVERS, IN HOME CARE
First Aid 101: What You Need to Know
First Aid 101
Knowing some basic first aid tips and techniques can equip you to react in an emergency situation and help loved ones.
What is First Aid?
First Aid is helping someone who is suffering from a sudden illness or injury. It can be a complete treatment such as applying ointment and bandages to a cut, or helping the individual with a more serious injury before they can get medical attention.
First Aid Tips: Proper first aid techniques can prevent a situation from escalating until a first responder arrives
- Be prepared: Have and know where the first aid kits are in your home, car and work.
- If an injury is serious, have someone call 911 while you help care for the victim.
- Learn the signs and symptoms of various illnesses including strokes and heart attacks.
Get First Aid Certified Today
The National Safety Council offers online training (source) and a list of local classes (source).
First Aid Basics
Bleeding
- Stop the bleeding as quickly as possible by applying direct pressure to the wound with a clean cloth
- Use a tourniquet if blood loss seems to life threatening. A belt or bandana can be used to pinch off the flow of blood.
- If the wound is very large, have the person lie down and elevate the part of the body that is bleeding.
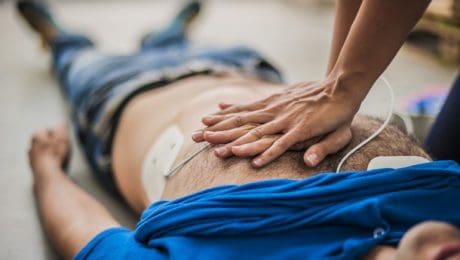
Having a Heart Attack
- Call 911
- Give the person an aspirin to help with potential heart damage.
- Perform CPR if the person stops breathing
Burned
- If the burn is mild, treat it by running it under cool water for 10 minutes.
- Then cover loosely with gauze.Never apply ice or ointment to the area.
- Call 911 if the burn is third– degree burns.
Choking
- A person who is choking cannot speak and will often clutch their hands to their throats.
- Try to make them cough by hitting your fist between their shoulder blades.
- Perform the Heimlich maneuver on them.
Signs of a Heart Attack
Signs of a heart attack include stab- bing chest pain, shortness of breath, fatigue, cold sweats, nausea, sudden dizziness, and chest discomfort.
First Aid Kit Checklist
Every home and workplace should have a First Aid Kit that is a well know location, accessible to everyone.
Anatomy of A First Aid Kit—What To Include In Yours (source)
- Absorbent compress dressings
- Various sized bandages
- Adhesive cloth tape
- Antibiotic ointment
- Antiseptic wipes
- Aspirin
- Breathing barrier (with one–way valve)
- Instant cold compress
- Non-latex gloves
- Hydrocortisone ointment
- Scissors
- Roller bandages
- Sterile gauze pads
- Oral thermometer
- Tweezers
- First aid instruction booklet
Check and Update Your Kit
- Check and replace flashlight batteries frequently
- Update emergency phone numbers
- Check the kit for refills regularly
- Check expiration dates on medications
Knowing proper first aid can help prevent bigger injuries and can help comfort an injured victim. Get certified today so you are prepared to help loved ones in a time of need.
Home Care Tip:
A “Caregiver First–Aid Kit” is an essential to home safety and care. Be sure your first–aid kit has all the critical supplies and is easily accessible to you at all times. Make a plan to check the kit regularly to discard and replace any expired or missing items.
- Published in CAREGIVERS, IN HOME CARE